Key Takeaways:
- Your child’s cancer care involves a full team, not a single doctor. A pediatric oncology care team typically includes oncologists, nurses, nurse practitioners, social workers, child life specialists, and other professionals who collaborate on every aspect of your child’s treatment and well-being.
- Each team member serves a distinct purpose. From the oncologist directing the treatment plan to the child life specialist helping your child cope through play, every role exists to address a specific medical, emotional, or practical need.
- Multidisciplinary care is linked to better outcomes. Research shows that children treated by coordinated, specialized teams at pediatric cancer centers have better survival rates and quality of life than those who receive fragmented care.
- You are part of the team too. Parents and caregivers play an active role in their child’s care, and knowing who does what helps you ask the right questions and advocate effectively.
When your child is diagnosed with cancer, you’re suddenly surrounded by new faces — doctors, nurses, specialists, and support staff — each introducing themselves with titles you may have never heard before. It can feel overwhelming. But every person on your child’s care team is there for a reason, and understanding who they are and what they do can help you feel more grounded during one of the most disorienting experiences a family can face.
A pediatric oncology care team is a group of specialized healthcare professionals who work together to diagnose, treat, and support children with cancer. Unlike adult oncology, pediatric cancer care requires providers trained specifically in how cancer behaves in growing bodies and developing minds — and how to deliver treatment in ways that protect a child’s long-term health, development, and quality of life.
At Cure 4 The Kids Foundation, Nevada’s only dedicated outpatient pediatric cancer and rare disease treatment center, this team-based approach is built into every aspect of care. Here’s who you’ll meet and what they do.

Who Is On a Pediatric Oncology Care Team?
A pediatric oncology care team brings together medical, psychological, and supportive care professionals under one coordinated plan. While the exact team composition varies by center and diagnosis, most pediatric oncology programs include the following core roles.
Pediatric Oncologist (or Pediatric Hematologist-Oncologist)
The pediatric oncologist is typically the physician leading your child’s cancer treatment. These doctors have completed specialized fellowship training in childhood cancers and blood disorders, which means they understand how pediatric cancers differ biologically from adult cancers and how to select treatments — including chemotherapy, immunotherapy, and targeted therapies — that account for a child’s growth and development.
Your child’s oncologist directs the overall treatment plan, orders and interprets diagnostic tests, coordinates with other specialists, and monitors your child’s response to treatment over time. At Cure 4 The Kids Foundation, board-certified pediatric hematologist-oncologists lead every patient’s care.
Nurse Practitioner (NP) or Physician Assistant (PA)
Advanced practice providers — nurse practitioners and physician assistants — work alongside the oncologist as part of the primary care team. They conduct physical exams, help manage symptoms and side effects, adjust medications, order labs, and often serve as a consistent point of contact for families between physician visits. For many families, the NP or PA becomes one of the most familiar and trusted faces in the clinic.

Pediatric Oncology Nurses
Pediatric oncology nurses provide direct, day-to-day patient care. They administer chemotherapy and other medications, monitor vital signs, manage central lines and ports, educate families on home care procedures, and watch for complications.
That said, the relationships they build with patients and families often make them one of the most trusted and familiar faces in the clinic. Research shows that oncology nurses are often among the first to notice signs of emotional distress in their patients — and that awareness is a critical part of the care chain, connecting families to the specialized behavioral health support they may need.
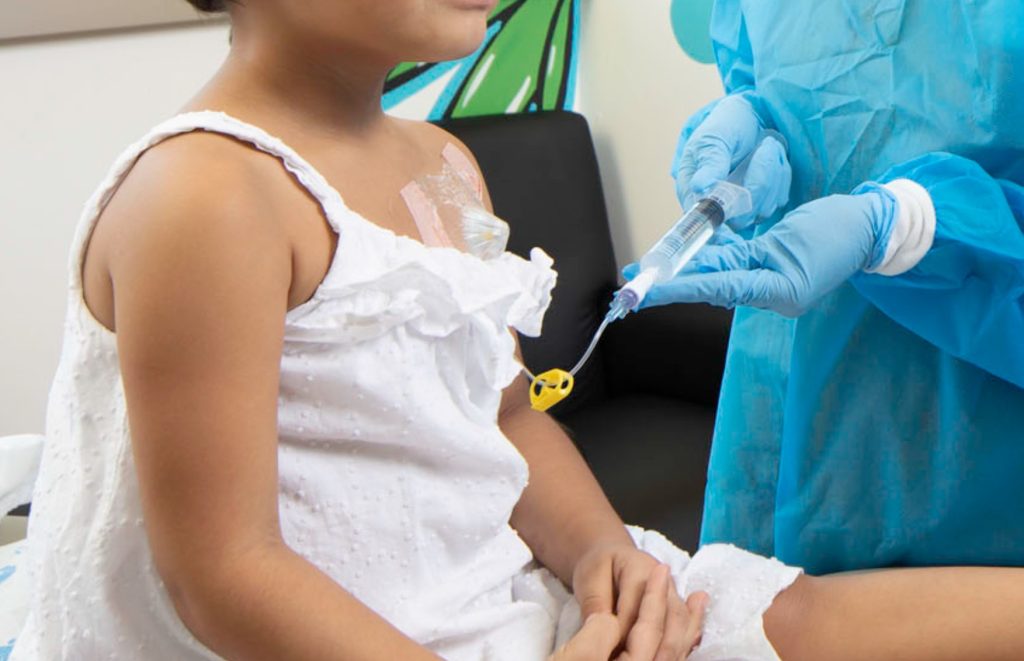
At Cure 4 The Kids Foundation, the nursing staff also specializes in complex and chronic infusion therapy, caring for patients whose treatments can range from a quick injection to a full-day infusion session.
Social Workers
Social workers are trained to address the practical and emotional challenges that come with a childhood cancer diagnosis. They conduct family needs assessments, connect families to community resources, help navigate insurance and financial assistance, provide therapeutic support, and intervene when safety concerns arise.
At Cure 4 The Kids Foundation, licensed social workers screen for family stressors, coordinate case management, and help assess patients who are transitioning to adult medical care, making sure no family faces these challenges alone.

Child Life Specialists
A certified child life specialist (CCLS) is a healthcare professional trained to help children understand and cope with the stress and anxiety of medical treatment. They use therapeutic play, age-appropriate education, and creative activities to help children process their diagnosis, prepare for procedures, and maintain a sense of normalcy during treatment.
For a 4-year-old, that might look like practicing with a cloth doll before a port access. For a teenager, it might mean having someone explain a treatment change in terms that respect their growing autonomy. Child life specialists also often provide support for siblings, who are often deeply affected by their brother’s or sister’s diagnosis.
At Cure 4 The Kids Foundation, child life specialists are on-site during infusions and treatments, bringing activities to the bedside and helping children find moments of comfort and even fun during long clinic days.
Clinical Neuropsychologist or Behavioral Health Provider
A cancer diagnosis affects more than the body. Clinical psychologists and behavioral health providers support the mental and emotional health of patients and their families throughout treatment. They screen for anxiety, depression, and trauma-related stress; provide coping strategies; and offer therapeutic interventions tailored to the developmental stage of the child.
Cure 4 The Kids Foundation’s Behavioral Health Department brings together neuropsychology, social work, and child life services under one coordinated program. The team participates in multidisciplinary case conferences, screens for safety risks, provides bereavement support, and ensures that psychological health is woven into every aspect of patient care.
Clinical Pharmacist
Clinical pharmacists play a critical behind-the-scenes role. They prepare and verify chemotherapy and other medications, calculate dosages appropriate for a child’s size and weight, monitor for drug interactions, and educate families on medication schedules and side effects. In pediatric oncology, where drug dosages must be precise and protocols are complex, the pharmacist is an essential safety check.
At Cure 4 The Kids Foundation, we have a pharmacy and pharmacists on-site so parents don’t have to travel to fill prescriptions for their kids somewhere else.

Radiologist and Imaging Technologist
Radiologists and imaging technologists use tools like X-rays, CT scans, MRIs, PET scans, and ultrasounds to help diagnose cancer, monitor tumor response, and guide treatment decisions. Some centers also have interventional radiologists who perform minimally invasive, image-guided procedures. These imaging specialists work closely with the oncology team to ensure the most accurate, up-to-date picture of your child’s condition.
Radiation Oncologist and Pediatric Surgeon
Depending on your child’s diagnosis and treatment plan, the care team may also include a radiation oncologist, who uses targeted radiation to shrink tumors and destroy cancer cells, and a pediatric surgeon, who performs biopsies, tumor removals, and other surgical procedures. Both of these specialists coordinate with the oncologist to time interventions for maximum effectiveness while minimizing impact on a child’s development.
Laboratory Team
The laboratory team processes blood samples, biopsies, and other diagnostic specimens that guide treatment decisions. Cure 4 The Kids Foundation’s on-site CAP-accredited laboratory (accredited by the College of American Pathologists) ensures that diagnostic results meet the highest standards for accuracy and reliability — a distinction shared by a select group of laboratories nationwide.
On-Site Educator
Many pediatric cancer centers recognize that treatment can disrupt months or even years of a child’s education. Some centers, including Cure 4 The Kids Foundation, address this through on-site classroom partnerships. C4K collaborates with the Clark County School District to provide continuity of education during treatment, helping children keep up with their schoolwork so they can transition back to the classroom more smoothly when they’re ready.

Why Does a Team Approach Matter in Pediatric Cancer Care?
Childhood cancer is not one disease — it encompasses more than a dozen major types and many more subtypes, each with its own biology, treatment protocols, and long-term considerations. No single provider can address all of these dimensions alone.
Research consistently shows that multidisciplinary team care improves outcomes for children with cancer. That’s why the Children’s Oncology Group (COG), which includes member institutions like Cure 4 The Kids Foundation that treat approximately 90% of children diagnosed with cancer in the United States, has established formal guidelines requiring multidisciplinary teams as a standard of care.
The overall five-year survival rate for childhood cancers in the United States has risen from 63% in the mid-1970s to 87% between 2015 and 2021. That progress is the direct result of collaborative, team-based approaches to research and treatment.
How Can Parents Work Effectively With Their Child’s Care Team?
You are a member of your child’s care team. It’s completely normal to wonder what to do when your child is diagnosed with cancer. Here are some practical ways to engage:
Ask each new provider to explain their role. It’s completely appropriate to say, “Can you tell me what you do and how you’ll be involved in my child’s care?”
Keep a notebook or digital file with names, roles, and contact information for every provider. During treatment, you’ll interact with many different people, and having a reference helps you direct questions to the right person.
Don’t hesitate to ask your social worker or patient navigator for help with anything outside of medical treatment — transportation, financial assistance, school accommodations, or emotional support. That’s exactly what they’re there for.
And remember to always speak up when something doesn’t feel right. Your knowledge of your own child is irreplaceable, and care teams rely on parents to report changes in behavior, appetite, energy level, and pain.
Frequently Asked Questions About Pediatric Oncology Care Teams
Who is the main doctor on a pediatric oncology care team?
The pediatric oncologist, also known as a pediatric hematologist-oncologist, typically leads the treatment plan and coordinates care among all other team members. This physician has specialized training in childhood cancers and blood disorders.
What does a child life specialist do in pediatric oncology?
A child life specialist is a certified healthcare professional who helps children cope with the stress and anxiety of cancer treatment. They use therapeutic play, age-appropriate education, and creative activities to help children understand their diagnosis, prepare for medical procedures, and maintain developmental progress during treatment.
Why is team-based care important for children with cancer?
Children with cancer have complex medical, emotional, and developmental needs that no single provider can address alone. Multidisciplinary teams coordinate treatment across specialties, which research has linked to improved survival outcomes, fewer complications, and better long-term quality of life for patients.
What is the role of a social worker in pediatric oncology?
Social workers in pediatric oncology help families navigate the practical and emotional challenges of a cancer diagnosis. This can include connecting families to financial assistance, providing therapeutic support, coordinating community resources, and conducting safety screenings.
Does my child need all of these specialists?
Not necessarily. The specific composition of your child’s care team depends on their diagnosis, treatment plan, and individual needs. Your child’s oncologist will determine which specialists should be involved and when.

About the Author: Annette Logan-Parker brings over 30 years of experience in pediatric oncology to her role as Founder and Chief Advocacy & Innovation Officer at Cure 4 The Kids Foundation. She has dedicated her career to improving outcomes for children with cancer and ensuring equitable access to cutting-edge treatments for all families.