Key Takeaways:
- Ask for a pediatric oncologist, not a general oncologist. Children are not small adults, and they need specialists trained specifically in childhood cancers.
- Write down your questions before every appointment. Bring a notebook or a trusted person to help you remember what the care team tells you.
- Seek a specialized pediatric cancer center with access to clinical trials, multidisciplinary care teams, and supportive services for the whole family.
- You are not alone. Social workers, patient navigators, family support programs, and parent communities exist to help you through this—and you deserve that support.

When the Doctor Says “Cancer”
Nothing can prepare you for hearing that your child has cancer. In that moment, the world narrows to a single, terrifying word, and everything after it becomes a blur. You may not remember what the doctor said next. You may not know what questions to ask. You may feel frozen, panicked, or numb.
All of that is normal.
If you are reading this at 2 AM because your child was just diagnosed—or because you are waiting for test results and bracing yourself—this guide is for you. I wrote it to help you understand what happens next, what questions matter most, and how to find the specialized care your child deserves.
You do not need to absorb everything at once. Bookmark this page. Come back to it. Share it with your partner, a grandparent, or a friend who is helping you navigate this. The information will be here when you are ready.
What Are the First Steps After a Childhood Cancer Diagnosis?
The hours and days immediately after a diagnosis can feel chaotic. Here is what to focus on first.
1. Breathe. You Have More Time Than You Think.
Many childhood cancers, while urgent, do not require treatment within hours of diagnosis. You typically have several days—sometimes a week or more—to gather information, ask questions, and begin to make informed decisions.
In fact, expert groups in pediatric oncology emphasize that a new diagnosis is overwhelming. Understanding all that is required from this point on is a process that will unfold for you over days and weeks, not just during one high-pressure conversation.
Your child’s medical team will let you know if your situation is an exception.
Right now, the most important thing you can do is be present for your child. They are watching you for cues about how to feel. You do not have to be strong. You just have to be there.
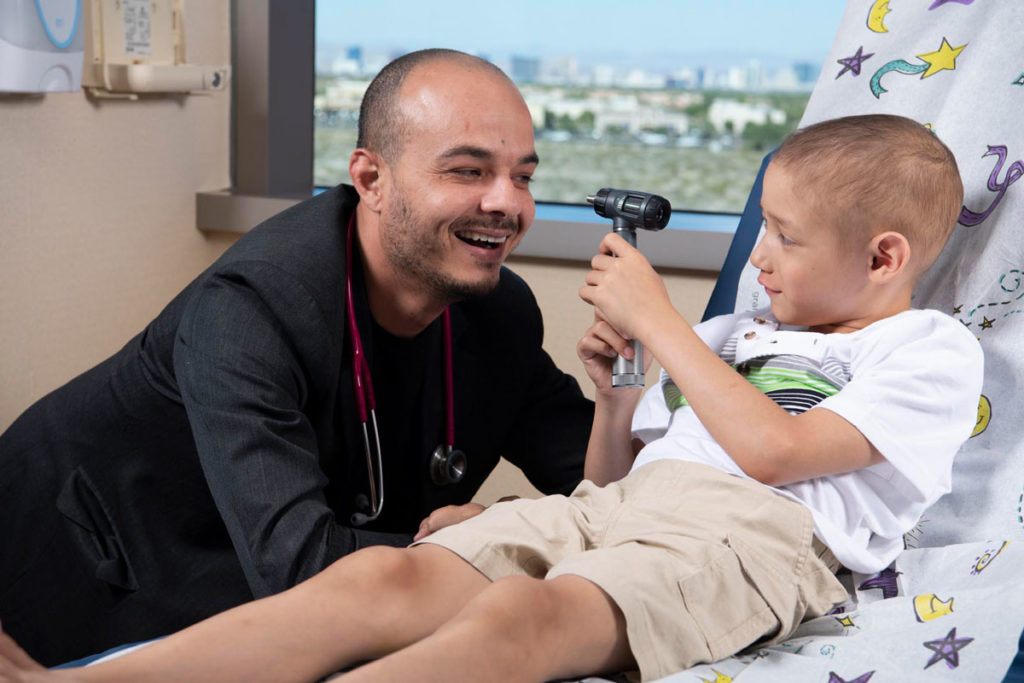
2. Make Sure You Have a Pediatric Oncologist
This is one of the most critical steps. A pediatric oncologist is a doctor who specializes exclusively in cancers that affect children and adolescents. Childhood cancers behave very differently from adult cancers—they respond to different treatments, grow at different rates, and require specialized protocols designed for developing bodies.
And, importantly, children with cancer who are treated at specialized, pediatric cancer centers have better survival outcomes than those treated in lower-volume or non specialty settings.
So, if your child was diagnosed at a general hospital or by a family pediatrician, ask for a referral to a pediatric hematologist-oncologist at a specialized children’s cancer center. This is not about doubting your current doctor. It is about making sure your child has access to the specific expertise their diagnosis requires.
3. Start a Medical Binder and a Digital Folder
From this point forward, you will be receiving a ton of medical information: lab results, scan reports, treatment plans, medication lists, and care instructions. Start organizing it now.
A simple three-ring binder and folder on your phone and/or computer can make a big difference. Be sure to include sections for diagnosis details, treatment schedules, medication names and dosages, insurance information, and contact numbers for your care team.
Many parents say this single step helped them feel more in control during an otherwise uncontrollable time.

What Questions Should I Ask My Child’s Oncologist?
You will have many appointments in the coming weeks for diagnostic tests, treatment planning, and care coordination. Having questions prepared helps you get the information you need and feel more active in your child’s care.
Here are the most important questions to ask early in the process:
About the Diagnosis
- What is the exact type and subtype of cancer my child has?
- What stage is the cancer, and what does that mean for my child specifically?
- Are additional tests or biopsies needed to confirm the diagnosis?
- Is this type of cancer common in children? What is the general prognosis?
About the Treatment Plan
- What treatment do you recommend, and why?
- What are the potential side effects—both short-term and long-term?
- How long will treatment last?
- Will my child need surgery, chemotherapy, radiation, or a combination?
- Are there clinical trials available for my child’s diagnosis?
About Daily Life During Treatment
- Can my child continue going to school? What accommodations might we need?
- What symptoms or side effects should prompt an emergency call or visit?
- Are there dietary changes or activity restrictions we should know about?
- What mental support services—social work, psychology, child life specialists—are available to us?
Do not worry about asking “too many” questions. Your child’s care team expects and welcomes them. If you think of questions between appointments, write them down so you do not forget.
What Should I Expect During My Child’s Cancer Treatment?
Every child’s treatment journey is unique, but understanding the general process can help reduce the fear of the unknown.
Diagnostic Phase
Before treatment begins, your child’s care team will run tests to determine the exact type, location, and extent of the cancer. This may include blood work, imaging scans such as CT, MRI, or PET scans, bone marrow biopsies, or surgical biopsies. This phase can feel like a difficult waiting period, but it is essential for developing the most effective treatment plan.
Treatment Planning
Once the diagnostic workup is complete, the oncologist will present a treatment plan. At a specialized pediatric cancer center, this plan is typically developed by a multidisciplinary team—a group of specialists that may include a pediatric oncologist, surgeon, radiation oncologist, pathologist, radiologist, social worker, psychologist, and child life specialist. This team approach ensures that every aspect of your child’s care is considered, from tumor biology to emotional well-being.
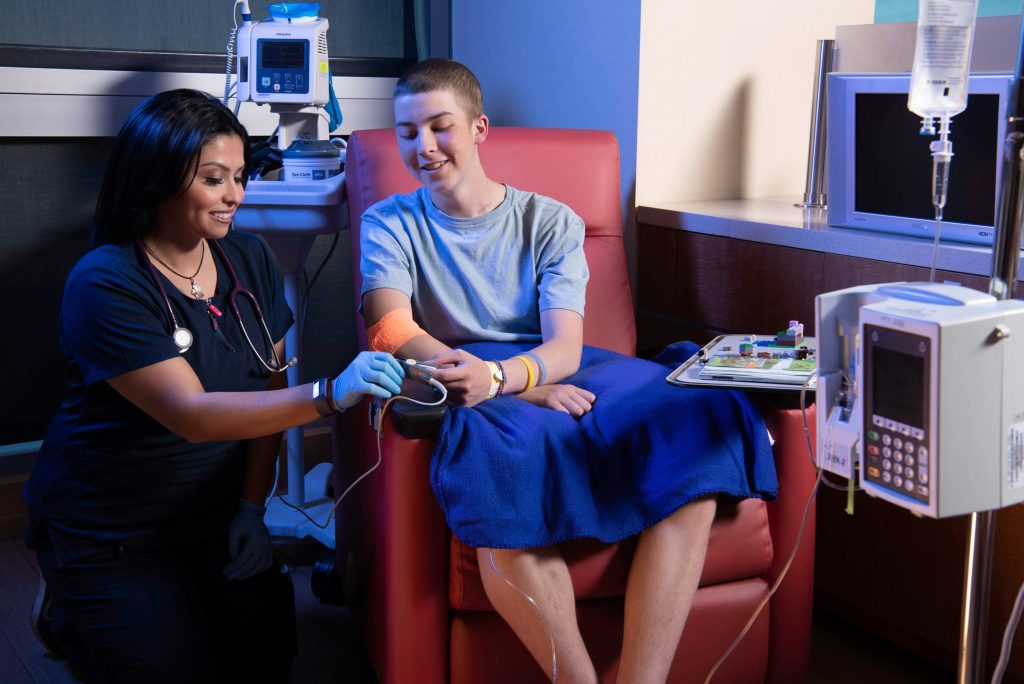
Active Treatment
Treatment may involve chemotherapy, surgery, radiation therapy, immunotherapy, targeted therapy, or some combination. The duration varies widely depending on the diagnosis—some treatment protocols last a few months, while others extend to two or three years.
During active treatment, your child may experience side effects like fatigue, nausea, hair loss, changes in appetite, or increased vulnerability to infections. Your care team will help you manage these side effects and will adjust the treatment plan as needed. Many children tolerate treatment better than parents expect, and your care team will work to maintain your child’s quality of life throughout.
Follow-Up and Survivorship
After treatment ends, your child will continue to see their oncologist for regular follow-up visits. These appointments monitor for any signs of recurrence and manage any long-term effects of treatment. Survivorship care is an important and ongoing part of your child’s journey, and a good pediatric cancer center will have programs specifically designed for childhood cancer survivors.
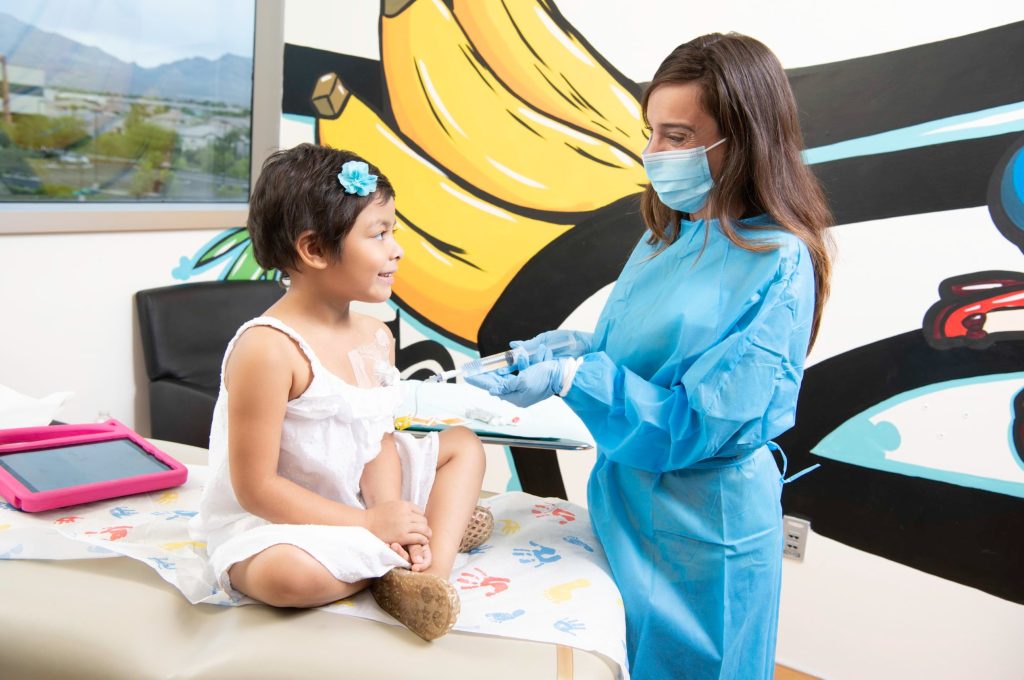
How Do I Find the Right Pediatric Cancer Specialist?
Not all cancer treatment centers are the same, and where your child receives care can make a meaningful difference in their experience and outcomes. Here is what to look for:
What Makes a Pediatric Cancer Center Different?
- Board-certified pediatric oncologists who treat childhood cancers exclusively—not adult oncologists who occasionally see children
- Multidisciplinary care teams that include specialists in surgery, radiology, pathology, psychology, social work, nutrition, and child life
- Access to clinical trials, which give children the opportunity to receive the newest and most promising treatments
- Family support services including financial counseling, social work, mental health support, and sibling programs
- Child-friendly environments designed to reduce fear and support the emotional needs of young patients
Why Specialized Pediatric Care Matters
Children are not small adults. Their cancers are biologically different from adult cancers, and the treatments that work for adults do not always work for children—and vice versa. Pediatric oncologists complete specialized fellowship training focused specifically on childhood cancers, and they follow treatment protocols developed through decades of pediatric-specific research.
Additionally, children’s developing bodies respond differently to treatments like chemotherapy and radiation. A pediatric specialist understands how to balance effective cancer treatment with minimizing long-term impacts on growth, development, fertility, and organ function.
How Do I Take Care of Myself and My Family Right Now?
When your child is diagnosed with cancer, every instinct tells you to focus entirely on them. But your well-being matters too—not as an afterthought, but as an essential part of your child’s support system.
Let People Help
If friends or family offer to bring meals, drive your other children to school, or sit with you during appointments—let them. Many parents feel guilty accepting help, but the people in your life want to support you. Consider setting up a meal train, a shared calendar, or designating one person as the “point of contact” who can relay updates to your wider circle so you do not have to repeat difficult information over and over.
Seek Emotional Support
A childhood cancer diagnosis affects every member of the family. Many pediatric cancer centers offer counseling for parents, therapeutic support for siblings, and child life services to help your child cope with their treatment. You may also find comfort in connecting with other parents who are going through—or have been through—a similar experience. Ask your child’s care team about parent support groups, both in-person and online.
If you notice yourself feeling persistently overwhelmed, unable to sleep, or struggling to function, please reach out to a mental health professional. You are going through one of the hardest experiences a parent can face, and you deserve support too.
Talk to Your Child Honestly
Children are perceptive. Even very young children can sense when something is wrong, and the unknown is often more frightening than the truth. Work with your child’s care team to find age-appropriate ways to explain what is happening. Honesty, delivered with reassurance, helps children feel safe and builds trust during a time when so much feels uncertain.
What About Insurance, Bills, and Financial Help?
The financial dimension of a childhood cancer diagnosis can feel almost as overwhelming as the medical one. Treatment is expensive, and even families with good insurance often face significant out-of-pocket costs.
Here is what to know:
- Talk to your hospital’s financial counselor or social worker immediately. They can help you understand your insurance coverage, identify financial assistance programs, and navigate billing.
- Ask about hospital charity care programs. Many pediatric treatment centers, including nonprofit organizations like Cure 4 The Kids Foundation, are committed to ensuring that no child is denied treatment because of a family’s inability to pay.
- Look into nonprofit and government assistance. Organizations such as the National Children’s Cancer Society, Alex’s Lemonade Stand Foundation, and state Medicaid programs (like CHIP) may provide financial support for families facing childhood cancer.
- Explore Family and Medical Leave Act (FMLA) protections if you need to take time off work to care for your child. Your employer’s HR department can walk you through your options.
Financial stress is real, and it is valid. But help is available, and you do not have to figure it out alone. Your child’s treatment center should have a dedicated team to help you navigate every aspect of the financial side.

Finding Specialized Pediatric Cancer Care in Nevada
If you are a family in Nevada, Cure 4 The Kids Foundation is the state’s only dedicated pediatric cancer and rare disease treatment center, and we currently employ 100% of Nevada’s board-certified pediatric oncologists. Located at 1 Breakthrough Way in Las Vegas, our clinic provides comprehensive cancer care for children and adolescents, from diagnosis through treatment and into survivorship.
Cure 4 The Kids Foundation’s care model includes board-certified pediatric oncologists, a full multidisciplinary team, access to clinical trials, behavioral health support, genetic counseling, and dedicated family support services. Our foundation was established in 2007 with a simple but powerful promise: no child with cancer will be turned away because of an inability to pay.
You Are Not Alone in This
A childhood cancer diagnosis changes everything, but it does not mean you are navigating this alone. From the medical team caring for your child to the social workers helping your family to the other parents who understand exactly what you are going through, there is a community of support waiting for you.
Take it one day at a time. Ask every question you have. Accept every hand that reaches out. And know that the strength you need is not something you have to find on your own.
It is something that will be built, day by day, by the people standing beside you.

About the Author: Annette Logan-Parker brings over 30 years of experience in pediatric oncology to her role as Founder and Chief Advocacy & Innovation Officer at Cure 4 The Kids Foundation. She has dedicated her career to improving outcomes for children with cancer and ensuring equitable access to cutting-edge treatments for all families.
Frequently Asked Questions
What is the first thing I should do when my child is diagnosed with cancer?
The first and most important step is to make sure your child is connected with a board-certified pediatric oncologist at a specialized children’s cancer center. Pediatric cancers require treatment protocols designed specifically for children, and a pediatric specialist has the training and experience to guide your family through this process.
How do I find a pediatric oncologist near me?
Ask your child’s pediatrician for a referral to a pediatric hematologist-oncologist. You can also search the American Society of Pediatric Hematology/Oncology (ASPHO) directory or contact a children’s hospital in your area. If you are in Nevada, Cure 4 The Kids Foundation is the state’s only dedicated pediatric cancer treatment center.
Is childhood cancer curable?
Many childhood cancers are highly treatable, and survival rates have improved significantly over recent decades. The prognosis depends on the type and stage of cancer, your child’s age and overall health, and the treatment plan. Your child’s pediatric oncologist can give you the most specific and accurate information for your child’s individual diagnosis.
How do I explain a cancer diagnosis to my child?
Work with your child’s care team, especially child life specialists, to find age-appropriate language. Be honest, be reassuring, and let your child ask questions at their own pace. Children generally cope better when they have some understanding of what is happening, even if the details are simplified for their age.
What financial help is available for families of children with cancer?
Many resources exist, including hospital charity care programs, nonprofit organizations like the National Children’s Cancer Society and Alex’s Lemonade Stand Foundation, state Medicaid programs, and federal protections like FMLA for work leave. Your hospital’s social worker or financial counselor is the best first point of contact for identifying programs available to your family.